Introduction
Although healing from a Chronic Illness, such a Chronic Fatigue Syndrome (ME/CFS) can be complex, basic principles will always form the foundations of a successful recovery journey. Sometimes the basics are almost too simple and can easily get overlooked in our search for answers or looking for more complex root causes.
Blood sugar stability of those basic principles and it if something that I end up refining with almost every client.
It is one of the pillars of the “Foundational Five Methodology“, the other four pillars being nervous system, sleep, pacing and managing inflammation (you can take the FREE Quiz, to identify which are most important for you).
Most people think;
“I eat a healthy diet and avoid refined sugars and processed foods”
“I have been to my GP and my blood tests suggest normal blood sugar”
“So therefore, my blood sugar is okay”
This may very well be true. However, clinical experience says, it often isn’t. Blood sugar imbalances can show up in subtle or unexpected ways throughout the day.
- Energy that changes after meals
- Losing function when you don’t feel hungry
- Waking in the middle of the night
- Craving carbohydrates and sugar
- Feeling irritable or lightheaded if meals are missed or delayed.
- A racing heart after a meal or autonomic symptoms when a meal is missed or imbalanced
And sometimes, an individual can lack the interoceptive awareness to connect how they are feeling to what they are eating, which means that they may not even be aware that they are experiencing symptoms. Because these symptoms can be subtle or inconsistent, they are not always easy to identify clearly
Which is why it is important to gather some objective data. This blog will help you to:
- Deepen your understanding about why blood sugar stability matters in Chronic Fatigue and other energy limiting conditions
- How to objectively assess blood sugar
- What to do about it
The Importance of Balanced Blood Stability in Fatigue Recovery
People who experience Chronic Fatigue, ME/CFS and energy limiting conditions or other complex illness are often sensitive to physiological and environmental changes. Small stressors can feel disproportionately overwhelming, there may be sensitivity to stimulation (light sensitivity, sound sensitivity etc.) or things completely fall apart after a bad night’s sleep – it all feels so much harder than a “normal” person.
The same can be true for seemingly benign changes in blood sugar.
Why Blood Sugar Fluctuations Can Feel More Significant In Chronic Fatigue
In someone with a more resilient system, normal fluctuations in blood sugar may come and go largely unnoticed. But in someone living with Chronic Fatigue, ME/CFS or another energy-limiting condition, those same shifts can feel much more significant.
This is partly because the nervous system is often already working with a reduced capacity to adapt to change. When the body perceives a drop in available energy, a missed meal, or a rapid rise and fall in blood sugar, this can act as a stress signal.
For someone who is already physiologically sensitive, that stress signal may be experienced as shakiness, irritability, lightheadedness, palpitations, anxiety, weakness, or a general sense of being less stable.
This does not mean the symptoms are psychological, and it does not mean the body is overreacting for no reason. It means the system is having to work harder to maintain stability.
In clinical practice, this is often why blood sugar stability can be so supportive. It is not just about glucose on a graph. It is about reducing unnecessary physiological stress, creating a steadier internal environment, and giving both the body and nervous system fewer reasons to become activated throughout the day.
To understand this more clearly, it helps to look at what is happening physiologically when we eat.
What Happens When We Eat?
When we eat, carbohydrates from food get broken down into sugars, absorbed through the digestive tract and blood sugar increases. A healthy body responds by producing insulin which takes sugar into cells and over a couple of hours, blood sugar returns to a steady baseline.
Most people feel unaffected by the rise and fall in blood sugar, however, in sensitive individuals, these physiological changes may have a more significant impact on how someone feels.
What may be considered a normal physiological response to a meal high in carbohydrate, could be a destabilising event for someone navigating a Chronic Illness.
What Works Better For Chronic Fatigue?
People who are sensitive to physiological fluctuations usually feel better when blood sugar fluctuates within a narrow range each day, without any highs and lows.
Although your GP may not be concerned with a post-meal blood sugar greater than 7mmol/L, generally I find that most people generally do better to keep their blood sugar below 6mmol/L after meals and no lower than 4 mmol/L between meals.
Here are some examples:
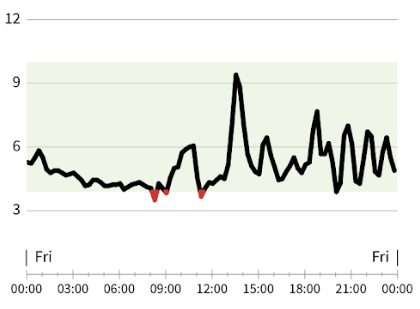
Example 1:
This is someone who experience quite extreme POTS. They struggle to eat but also struggle to not eat. This keeps them on a rollercoaster of ups and downs each day – when meal choices are not optimal.
Although their blood sugar is technically “in range” most of the day, what we notice by using a continuous glucose monitor (CGM), is the rapid transitions (the rapid increase followed by rapid decrease). It is this exact pattern which can be both destabilising for blood sugar and the nervous system.
Both high and low blood sugar negatively impact energy production. High blood sugar means that glucose isn’t getting into the cells where it can be converted to energy.
When blood sugar drops low again, the body experiences the physiological shift. As blood sugar rapidly drops, the nervous system becomes more activated and cortisol is released to bring stored fuel into circulation.
This is a common pattern that I see in many clients even when their bloodwork suggests that sugar levels are normal. In the early stages of recovery, stabilisation is key and the use of the continuous glucose monitor enables us to identify real time patterns in response to food and from here, we can optimise diet and create more stability.
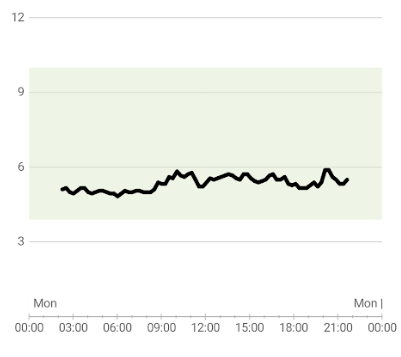
Example 2
This is an example of what can be achieved when the right dietary strategy is applied.
When Blood Sugar Imbalances Aren’t Just About Sugar
When we talk about blood sugar, it is easy to focus only on what we are eating. But in clinical practice, we often see that blood sugar instability is not just about sugar or carbohydrates alone.
How much you eat, how often you eat, and how consistently you fuel your body can all play a significant role.
Many people living with Chronic Fatigue or energy-limiting conditions unintentionally under-eat. This can happen for a number of reasons such as restrictive diets, reduced appetite, digestive discomfort, fatigue making food preparation more difficult, or sometimes fear that certain foods may worsen symptoms.
Over time, low or inconsistent energy intake can place additional strain on the system. If the body is not receiving enough fuel, or meals are spaced too far apart, blood sugar may drop more easily. In response, the body may increase stress hormones such as cortisol to bring stored energy into circulation.
This can contribute to symptoms such as feeling wired but tired, shaky, lightheaded, irritable, or experiencing dips in energy that feel difficult to recover from.
Irregular eating patterns can have a similar effect. Skipping meals, delaying food for long periods, or having very uneven meal sizes across the day can make it harder for the body to maintain stability.
In many cases, before making significant changes to what someone is eating, we start by supporting how they are eating. This might include:
- Eating consistently throughout the day
- Ensuring meals are sufficiently nourishing
- Reducing long gaps between meals where possible
For some people, this alone can begin to create a more stable foundation.
A Note on Individualisation and Starting Point
Before making significant changes to your diet, it is important to recognise that there is no single approach that works for everyone.
In clinical practice, we rarely begin with highly restrictive protocols. While some individuals may benefit from reducing certain foods, more restriction does not necessarily lead to better outcomes — and in some cases, it can make things more difficult.
For many people, the most supportive starting point is not removing large numbers of foods, but first creating stability. This often means:
- Eating regularly
- Ensuring meals are sufficiently nourishing
- Building meals that include protein, fats and fibre
From this foundation, adjustments can then be made gradually and in a way that is guided by your individual response.
It is also important to ensure that overall food intake remains adequate. Reducing foods without appropriately replacing them can lead to unintentional under-eating, which may further impact energy, blood sugar stability and overall resilience.
The goal is not to create a perfect diet, but to create a way of eating that supports stability, feels sustainable, and works with your body rather than against it.
Guidelines for a Foundational Strategy
The exact right approach for each individual may look slightly different. However, very simply, the following is a useful framework to follow:
- Plan meals around animal protein offering 30-40g of protein per meal -this is approximately 150g – 200g raw poultry, fish or meat
- Ensure adequate fibre intake by eating two cupped handfuls of low carbohydrate vegetables with eat meal
- Consume adequate fats from avocado, olive oil, olives, nuts and seeds, butter or coconut (milk, butter, cream, yoghurt)
- Consume carbohydrates to tolerance; this is where things may need to be more personalised
How Much Carbohydrate Should I Eat?
There is no exact carbohydrate prescription that works best for everyone. Some of my clients find a ketogenic diet most effective, where others prefer to keep small amounts of carbohydrate in their diet.
In clinical practice, we rarely begin with full restriction. For many people, stabilising meals first — before removing large food groups — is often more supportive.
When someone is physiologically sensitive, it is best to avoid big or sudden changes.
Therefore, I prefer to suggest “crowding in” first with proteins, fats and fibre. And then gently adjusting carbohydrates as follows while using a CGM to monitor glucose responses.
- Adjust or remove refined sugars (sugar, honey, coconut sugar and other alternatives, sweets)
- Adjust or remove refined grains (e.g. white flour, white rice)
- Adjust or remove grains and white potato
- Adjust or remove fruits apart from low sugar fruits like melons and berries
- Adjust or remove beans and pulses (edamame beans will be okay if soy is tolerated)
- Adjust or remove sweet potato
- Adjust or remove butternut squash, carrot, beetroot and any other root vegetables
- Adjust or remove all fruits
These are progressive options, not requirements and therefore it is worh noting:
- How someone responds to food is highly individual. Some people may feel well removing foods 1-2, others may need to work all the way from steps 1-8.
- Sometimes some foods are tolerated better than others e.g. white potato may be okay not not carrots
- When removing foods from your diet, we must make sure that calorie intake is stable across the day to avoid unintentional blood sugar lows. This might mean increasing protein, fat and fibre further to compensate.
What Else Matters
In addition to what you eat it is important to note that how much and when you eat also matters. People who are physiologically sensitive respond well to rhythm and routine. This means you may want to:
- Eat at the same time(s) each day
- Evenly distribute calories across all meals – many people tend to eat too little earlier in the day and too much in the evenings
- Eat as often as needed to stay stable – for some people this may be every 2 hours, for others, every 4-5 hours is just fine
- Hydrating adequately and distributing hydration across the day may also be supportive
- While stability is the goal, avoiding caffeine is recommended or if you must have caffeine, have it after a satiating meal and never later than 12pm, depending on your biorhythm.
Bringing It All Together
If you are feeling overwhelmed reading this, that is completely understandable. There are many moving parts when it comes to health, and it is easy to feel like you need to change everything at once.
In reality, this is rarely helpful.
In most cases, the most supportive approach is to start small and build gradually. This might simply mean beginning to notice how you feel after meals, creating a little more consistency in when you eat, or ensuring your meals feel more nourishing and balanced.
You do not need to have a perfect diet to begin seeing changes. Small shifts, applied consistently, can begin to create a more stable foundation over time.
It is also important to remember that blood sugar is just one piece of a much bigger picture. Factors such as sleep, nervous system regulation, pacing and inflammation all interact with one another, and it is often the combination of these that shapes how someone feels day to day.
If you recognise yourself in some of the patterns described in this blog, take that as information – not as something you need to fix immediately. Your body is not working against you. It is responding to its current environment and capacity.
With the right support, and by working with your body rather than against it, it is possible to create more stability over time.












